
SKIN ULTRASOUND
The dermatologic ultrasound web site
NEWS !!!
-Breaking News !!! Follow us on Instagram, Twitter and Facebook
-New!!! High-frequency Ultrasound of Genodermatoses
-New!!! Ultrasound of Lip Anatomy and Filler Placement!
–New!!! Ultrasound- Guided Hyaluronidase for Managing Vascular Occlusions
–New!!! Artificial Intelligence Deep Learning Discrimination of Cosmetic Fillers
-New!!! Hidradenitis Suppurativa at The Lancet
–New !!! Scoring for Assessing the Degree of Inflammation in Hidradenitis Suppurativa- Modified US-HSA
New!! International Multicentric Study on Granulomas after Cosmetic Filler Injections
–New!!! International Consensus on Ultrasound in Aesthetics
–New !!! International Consensus on Ultrasound of HS
New!!! Ultrasound in Skin Cancer: Why, How and When to Use it
–New!!! Full issue dedicated to Dermatologic Ultrasound of the Journal Seminars in Ultrasound, CT and MRI
–New!!! Ultrasound Patterns of Vitiligo at High and Ultra-High-Frequency
–Modified US-MAS scoring for assessing the activity of morphea over time
–Concepts, Role and Advances on Nail Imaging
–Color Doppler ultrasound: A Standard of Care in Hidradenitis Suppurativa
–Ultrasound of the Hair, Sebaceous Glands and Apocrine Glands

Useful Information
-Check Color Doppler ultrasound assessment of morphology and types of fistulous tracts in hidradenitis suppurativa (HS)
– Check Accuracy of Ultrasound on Location of Lipomas in Forehead
-Check article on Ultrasound Diagnosis and Staging in Pediatric Hidradenitis Suppurativa
-Check the post Trust: The Passport on Imaging of the Skin
–First Guidelines for Performing Dermatologic Ultrasound
-Check the AIUM official blog How I Became Involved in Dermatologic Ultrasound
-Follow and join the discussion and the comments on the wall on AIUM dermatologic ultrasound interest group
-Follow us on Twitter and our Facebook Page Skin Ultrasound

Dealing with Epidermal Cysts: Dream or Nightmare?
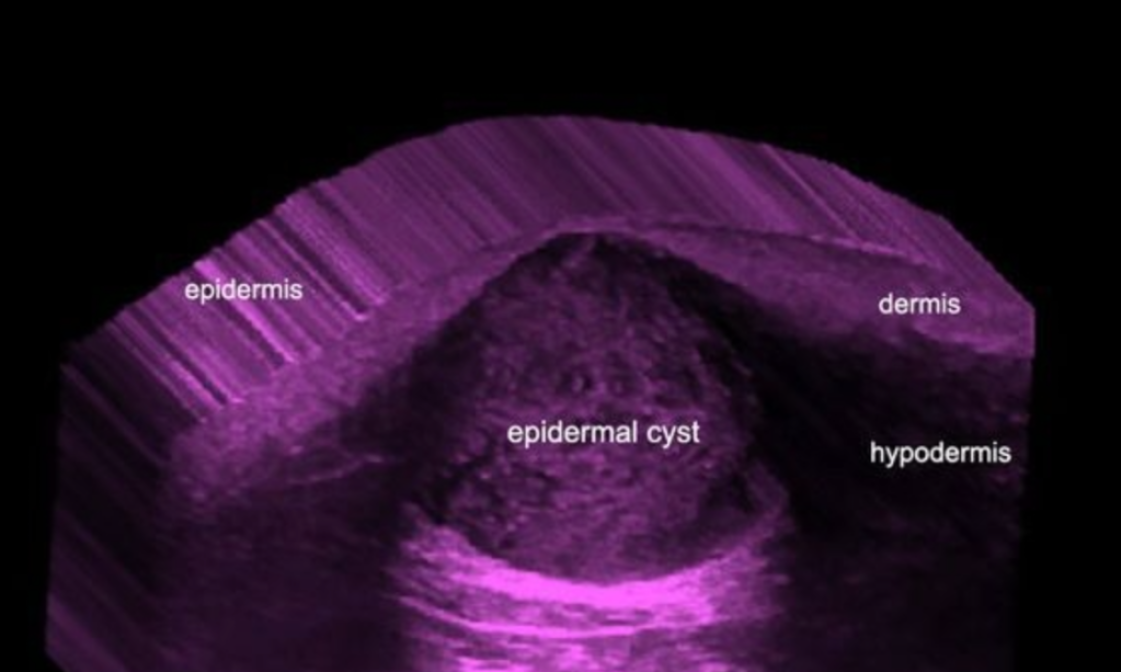
These cutaneous cysts are generated by the implantation of epidermal components in the dermis and subcutaneous tissue. Thus, the causes can be embryonic, traumatic or secondary to surgical procedures. Epidermal cysts are covered by stratified squamous epithelium with a granular layer. Hence, the name «sebaceous cyst» is a misnomer and may be confusing.
Clinically, they usually show as erythematous and sometimes painful nodules, often with a small opening on the surface, also called “punctum” which correspond to the communication of the cyst with the epidermal layer. These cysts may drain foul smelling and cheesy-like material and contain keratin, cholesterol and sometimes calcifications.
One of the problems with epidermal cysts is that they can be potent simulators of other lesions, especially when the wall of the cyst ruptures and the cyst become inflamed. Therefore, they can mimic pilomatrixomas, dermatofibromas, foreign bodies, among other lesions. Furthermore, to prevent recurrence, the wall of the cyst (that generates the keratin) should be completely removed.
On sonography, they show a variable appearance according to the phase of the cyst. If they are intact, the sonograms will usually show a well defined, rounded- or oval shaped, anechoic or hypoechoic structure located in the dermis and subcutaneous tissue. Also, these cysts may present inner echoes (debris) and sometimes show a “pseudotestes appearance” ( ie. brighter inner echoes and anechoic filiform areas) as the result of highly compacted deposits of keratin and cholesterol. Commonly, a connecting anechoic tract (punctum) to the epidermis can be detected on ultrasound.
Nevertheless, when the cyst is complicated with a rupture, the keratin is spread into the surrounding tissue and elicits inflammation and a foreign body reaction. The latter events may cause hypoechoic collections, adjacent to the cysts or a big change in the morphology of the cysts that turn into ill-defined hypoechoic structures.
Interestingly, posterior acoustic enhancement, a classical artifact of the cystic lesions, is usually conserved during all the phases. Ultrasound can show the lesion and measure the extent in all axes as well as demonstrate the connecting tracts and perform the differential diagnosis with other conditions. Moreover, color Doppler ultrasound may show increased blood flow in the periphery of the cysts during the phases of inflammation and rupture, frequently with low- flow vessels.
The proper recognition and assessment of the extent of these cystic entities through the sum of the clinical and anatomical data provided by sonography may support an early diagnosis and proper treatment. Thus, the addition of the ultrasound technology perhaps may help to deal with these entities, turning a possible nightmare into a dream.
References
1-Huang CC, Ko SF, Huang HY, Ng SH, Lee TY, Lee YW, Chen MC.Epidermal cysts in the superficial soft tissue: sonographic features with an emphasis on the pseudotestis pattern.J Ultrasound Med. 2011;30:11-7.
2-Jin W, Ryu KN, Kim GY, Kim HC, Lee JH, Park JS. Sonographic findings of ruptured epidermal inclusion cysts in superficial soft tissue: emphasis on shapes, pericystic changes, and pericystic vascularity. J Ultrasound Med. 2008;27:171-6
3-Kuwano Y, Ishizaki K, Watanabe R, Nanko H. Efficacy of diagnostic ultrasonography of lipomas, epidermal cysts, and ganglions. Arch Dermatol. 2009 ;145:761-4.
4-Wortsman X, Wortsman J, Clinical usefulness of variable frequency ultrasound in localized lesions of the skin. J Am Acad Dermatol 2010; 62 : 247-256
5-Wortsman X.Common applications of dermatologic sonography.J Ultrasound Med. 2012 ;31:97-111
Pilomatrixomas: Masters of Disguise ?
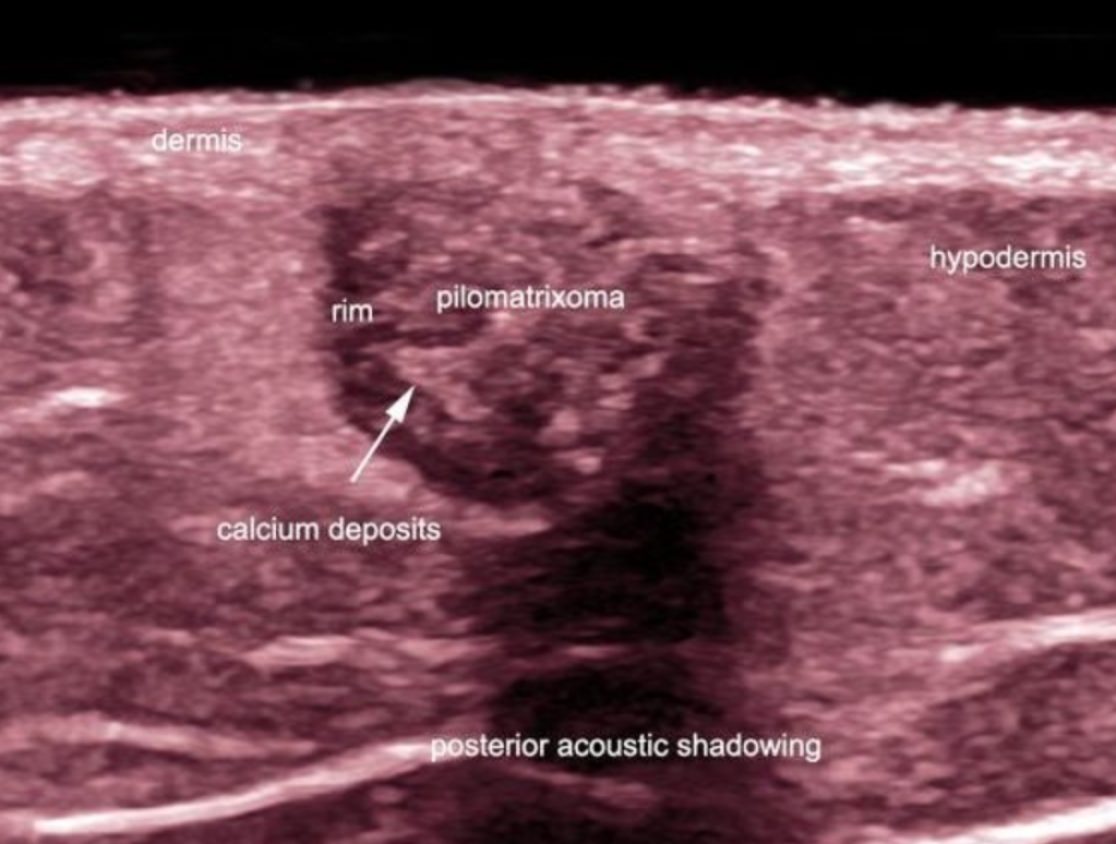
Pilomatrixomas, also called pilomatricomas or calcifying epitheliomas of Malherbe are common and benign skin tumors that arise from the hair follicle matrix. These conditions are more common in children and young adults, especially on the head, neck and extremities. Clinically, they usually present as single or multiple painless, erythematous or slightly bluish nodules. Thus, these tumors can easily mimic other cutaneous lesions such as epidermal cysts, foreign body reactions, fat necrosis, calcified lymph nodes or vascular tumors, among others, on the clinical examination. Moreover, clinical misdiagnosis has been reported as high as 54% in some series.
On sonography, pilomatrixomas classically appear as target-shaped nodules with well-defined hypoechoic rim and hyperechoic center. Scattered hyperechoic dots producing posterior acoustic shadowing that correspond to calcium deposits may be found within the nodule nucleus (partial calcification). Nevertheless, 15 to 30% of pilomatrixoma cases had been reported to not show calcium and 45 % of these entities, in other series, had been reported as completely calcified. Furthermore, there are rare cystic variants of pilomatrixomas. On the other hand, variable degrees of vascularity can be present within the tumor which may also explain the challenging clinical diagnosis.
Ultrasound had reported correctness of diagnosis from 76% to 96% and provides reliable information about the extension, location and blood flow of the lesions. Therefore, a pre-surgical sonographic examination may be a good tool for removing the clinical disguise of these tumors.
References
1-Roche NA, Monstrey SJ, Matton GE. Pilomatricoma in children: common but often misdiagnosed. Acta Chir Belg. 2010 ;110:250-254.
2-Kumaran N, Azmy A, Carachi R, Raine PA, Macfarlane JH, Howatson AG. Pilomatrixoma–accuracy of clinical diagnosis. J Pediatr Surg. 2006 ;41:1755-1758.
3-Choo HJ, Lee SJ, Lee YH, Lee JH, Oh M, Kim MH, Lee EJ, Song JW, Kim SJ, Kim DW. Pilomatricomas: the diagnostic value of ultrasound. Skeletal Radiol. 2010;39:243-250.
4- Solivetti FM, Elia F, Drusco A, Panetta C, Amantea A, Di Carlo A. Epithelioma of Malherbe: new ultrasound patterns. J Exp Clin Cancer Res. 2010 6;29:42.
5-Wortsman X, Wortsman J, Arellano J, Oroz J, Giugliano C, Benavides MI, Bordon C. Pilomatrixomas presenting as vascular tumors on color Doppler ultrasound. J Pediatr Surg. 2010;45:2094-2098.
6-Wortsman X.Common applications of dermatologic sonography.J Ultrasound Med. 2012 ;31:97-111



FACTS
-More than 100,000 visitors from more than 150 countries and from the 5 continents
-More than 280 references about dermatologic ultrasound
International Patients check here
Double Reading check here
SKIN ULTRASOUND

The last 23 years have marked an interesting road in the development of the dermatologic ultrasound.
An explosive growth has been seen due to the need for non-invasive studies of the skin and nails. Physicians and patients demand anatomical studies that match clinical signs for optimal medical and surgical planning as well as excellent cosmetic results.
In this web site, you will find images, references and links that may help you understand and/ or develop this exciting new tool at your own work place.
My best wishes to you and your team
Ximena Wortsman MD, FAIUM
Fellow Member at AIUM ( American Institute of Ultrasound in Medicine)
Department of Imaging, IDIEP-Institute for Diagnostic Imaging and Research of the Skin and Soft Tissues
Adjunct Associate Professor
Department of Dermatology
Faculty of Medicine, Universidad de Chile
Adjunct Professor
Department of Dermatology
School of Medicine
Pontificia Universidad Católica de Chile
Address:
IDIEP
Lo Fontecilla 201, of 734,
Las Condes, Santiago, Chile
Phone:+56222446058
WhatsApp IDIEP
+56992505421 / +56941164873
e-mail: skinultrasound@gmail.com
Links to this web page are available in
facebook.com/RSNAfans
facebook.com/pages/American-Institute-of Ultrasound- in- Medicine- AIUM
dermweb.com/dermatology_resources/external.htm#Journals
SEUS.org/enlaces(Spain Ultrasound Society)
facebook.com/radRounds
Ximena Wortsman
www.ximenawortsman.com
Address: Lo Fontecilla 201, of 734, Las Condes
Santiago
Chile
Phone: +56222446058
Copyright© Ximena Wortsman – 2026